Our service covers the full cycle billing, corrections, and securing your revenue.
It’s time to turn your medical billing into a reliable revenue stream. Our certified billers bring over 20 years of expertise in coding, compliance, and claims management ensuring accuracy in every detail, from ICD, CPT, and HCPCS codes to proper modifiers and strict HIPAA compliance. Every claim is carefully reviewed before reaching the payer, helping us achieve a 99% first-pass approval rate.
Experience the impact of accuracy on your revenue growth.
Our team reviews your billing process, identifies revenue leaks, and eliminates them at the source—ensuring predictable revenue and smooth cash flow without the hassle of follow-ups.
RCM Services
Outcomes That Matter More Than Promises:
Key performance metrics driving United State most dependable medical billing agency
Trusted solutions for medical billing success
- AR reduced to under 30 days
- 20–25% increase in revenue
- 99% first-pass acceptance rate
- 96% collection rate
- 98% clean claims submission rate
Supporting United State's healthcare providers, from solo practitioners to surgical centers.
Every healthcare provider faces unique billing challenges, and we handle them accordingly. Whether you are running a small clinic or managing hospitals, we provide medical billing services to every specialty.
Small Practices or Solo Providers
Hospitals and Health Systems
Physicians from Every Specialty
- Our medical billing support reduces costs and speeds up payments without extra overhead.
- Our United States expert medical billers deliver ASC-focused compliant coding for faster, accurate reimbursements for Ambulatory Surgical Centers.
- Rapid billing support for urgent care and walk-in clinics that matches your patient flow and ensures timely reimbursements.
- Our United States medical billing services provide specialty-specific coding that captures every dollar you deserve.
- As one of the leading medical billing and coding companies, we deliver streamlined billing that saves time, reduces costs, and accelerates payments.
- We simplify billing workflows for group practices to ensure smooth and steady reimbursements.
RCM Services
Keep your billing transparent, predictable, and easy to understand.
We keep providers informed at every step—from claims submission to payment posting—through transparent reporting, real-time tracking, and full visibility into the revenue cycle. With advanced billing systems and strict data security protocols, Doctor Management Services goes beyond billing. We act as your dedicated partner in financial growth, ensuring every claim brings you closer to success.

Full Transparency
Real-Time Billing Insights
Billing Audits
- Our medical billing support reduces costs and speeds up payments without extra overhead.
- Our United States expert medical billers deliver ASC-focused compliant coding for faster, accurate reimbursements for Ambulatory Surgical Centers.
- Rapid billing support for urgent care and walk-in clinics that matches your patient flow and ensures timely reimbursements.
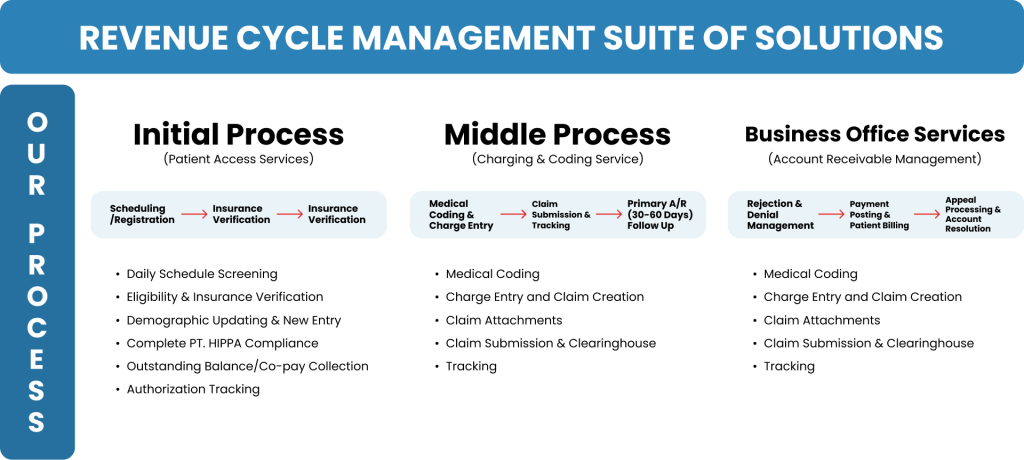
Strengthen Your Revenue Cycle with Our Expert Medical Billing Solutions
At GPA Consultancy, we specialize in optimizing your revenue cycle through, expert complete medical billing services. From small practices to large hospitals, we understand the intricate world of medical billing and its critical role in your healthcare organization.
Our dedicated team of experts is committed to simplifying the billing process, maximizing your revenue, and allowing you to prioritize exceptional patient care. With skilled account managers and advanced medical billing software, we streamline everything from electronic claims submission to payment follow-up, ensuring a cost-effective solution that boosts your bottom line.

Improve Your Medical Billing Process with Ease
Experience seamless and efficient medical billing services with Gpa Consultancy. Our dedicated team works hand-in-hand with your healthcare professionals to integrate our expert billing knowledge with your organization’s unique insights. This collaborative effort fosters a dynamic synergy, continuously enhancing and optimizing your billing procedures. We aim to streamline your billing operations, ensuring smoother processes and improved outcomes.
Our Services:
Insurance Benefit Verification
Medical Coding
Claim Submissions & Follow-up
Denial Management
Accounts Receivable (A/R) Management
Reporting & Analytics

The Key Components Within Our Comprehensive Medical Billing and Coding Services
Revenue Leakage Analysis
- Through Coding and Benchmarking
- Error trend detection and analysis
- Immediate corrective measures implemented
- Preventive action plans for ongoing improvement
Improvements to Clean Claims %
- Diligent measuring and analyses of data
- Easily digestible reporting offered to teams
- Ongoing improvement actions taken
Revenue Leakage Analysis
- Through Coding and Benchmarking
- Error trend detection and analysis
- Immediate corrective measures implemented
- Preventive action plans for ongoing improvement
Improvements to Clean Claims %
- Diligent measuring and analyses of data
- Easily digestible reporting offered to teams
- Ongoing improvement actions taken
Advance Reports & Analytics
- Custom Reports and Analytics: Leverage measurable performance data and prebuilt integrations with top EMR systems.
- Advanced Visualization: Access advanced visualization tools for creating reports and interactive dashboards.
- Stay Informed: Monitor key performance indicators relevant to your revenue cycle, enabling proactive decision-making.
- Seamless Integration: Enjoy seamless integration with EMR systems, eliminating manual data entry and ensuring data accuracy.
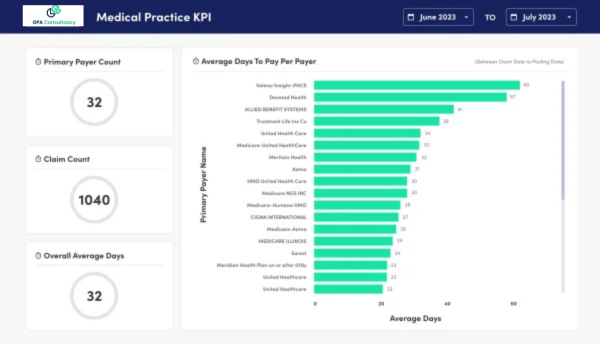
Transform Your Revenue Cycle: Drive Results with Medical Billing and Coding Solutions
At GPA Consultancy, we are experts in medical billing and coding services. We focus on optimizing the entire billing process for sustained financial growth and operational excellence.

Featured Billing Success Story
End-to-End Services, One Expert Partner.
With over years of end-to-end healthcare operations expertise, GPA Consultancy brings a broader perspective that goes beyond isolated solutions.
- Finance
- Marketing
- Operations
- Clinical Support

Payer Contract Rate Negotiation
Optimize reimbursement rates and improve financial outcomes.
Revenue Cycle Management (RCM)
Enhance revenue and efficiency through our end-to-end RCM expertise.
Medical Licensing
Ensure compliance and quality care with provider and organizational medical licensing services.
Medical Coding Audits
Enhance accuracy and compliance in healthcare organizations.
Credentialing
Prevent operational hiccups and cash-flow obstacles by keeping all your providers billable.
Bookkeeping Outsourcing
Manage accounts with our R2R and P2P solutions.
Medical Billing & Coding
Prevent revenue loss and non-compliance with our expert teams.
Forecasting and Analytics
Leverage insights for informed decision-making.

Digital Marketing and Branding
Elevate your brand presence and attract patients.
Social Media Management
Engage with your audience and drive growth through effective advertising.
Reputation Management
Monitor and enhance your online reputation.
Marketing Analytics
Track and measure the success of your campaigns.
Website Design and SEO
Build a user-friendly website optimized for search engines.

Credential Verification Organization (CVO)
Streamline credentialing processes.
Phone Triage and Contact Center Operations
Enhance patient communication and engagement.
Patient Access Services
Optimize intake, scheduling and administrative functions.
Patient Satisfaction Initiatives
Implement strategies to improve the patient experience.
Benefit Verification and Prior Authorizations
Ensure smooth patient flow and satisfaction.

Provider Recruitment
Attract and retain top talent for your organization.
Utilization Management
Enhance care delivery through effective resource management.
Medical Scribes
Improve documentation efficiency and accuracy.
Clinical Appeals
Navigate the appeals process with expert support.
Care Coordination
Support Remote Patient Monitoring (RPM), Chronic Care Management (CCM), and Remote Therapeutic Monitoring (RTM).
Why Choose GPA Consultancy Medical Billing Solutions?
Our experts are skilled at efficiently submitting claims, ensuring accurate coding, and promptly following up on accounts receivable.
Our teams have specialized knowledge in CPT and ICD-10 coding, which helps reduce the number of denied claims.

- Expertise and Accuracy: Access to specialized skills and expertise in medical billing, ensuring accurate coding and claims submission.
- Maximized Revenue: Professional billing services are adept at optimizing revenue cycles, minimizing claim denials, and ensuring timely payments.
- Saves money: No need for staff, training, or overhead for billing infrastructure.
- Efficiency and Productivity: Streamlines processes, leading to increased efficiency and productivity in the practice.

- Adherence to Compliance: Ensures compliance with constantly evolving healthcare regulations, reducing the risk of legal issues and penalties.
- Less billing errors: Uses advanced technology and skilled professionals, resulting in fewer claim rejections.
- Faster Payments: Accelerates the payment cycle by submitting claims promptly, resulting in quicker reimbursement for services rendered.
- Scalability: This allows for flexibility to meet the changing needs of the practice, whether it’s growing or seeing more patients.
Go Beyond Billing and Coding and Take Complete Ownership of Your Revenue Cycle
Create a high-performing collections process synergy with services designed to collaborate and complement
each other to minimize financial losses and maximize the overall patient experience.

Licensing Service

Credentialing Services

Insurance Contract Negotiation

Scalable Services
RPA & API Proficiency

Flexible Pricing Options
Specialty-Specific Medical Billing and Coding Services
GPA Consultancy is a multi-specialty medical billing services company in the USA with over 12 years of experience. We assist medical practices nationwide, including Texas, California, New York, Hawaii, and more. Our team specialize in maximizing billing claims payments in all 50 states, securing financial success for our clients. GPA Consultancy is a multi-specialty medical billing services company in the USA with over 12 years of experience. We assist medical practices nationwide, including Texas, California, New York, Hawaii, and more. Our team specialize in maximizing billing claims payments in all 50 states, securing financial success for our clients.

Mental Health

General Surgery

Orthopedic
Nephrology

ENT

OBGYN
Gastroenterology

Pediatric
Our medical billing procedure workflow:
Every stage of your billing process, from benefits verification to denial management, is managed by certified experts to ensure compliance, transparency, and full reimbursement. The Doctor Management Services redefines your medical billing experience through improving profitability, converting more A/R to cash, and working more efficiently.
Verification of Benefits (VOB)
We know accuracy matters; that’s why we start with accuracy at the very first step. By verifying each patient’s insurance coverage. Our team first checks each patient’s eligibility, deductibles, and authorization requirements before the appointments by calling or checking on the insurer’s website. After verifying benefits in advance, it reduces the chances of errors, avoids delays, and claim rejections.
Patient Demographics Entry
Even a single digit entered incorrectly in the documentation can hold up a claim. Our California expert billing team carefully enters and validates patient demographics to ensure everything, from policy numbers to date of birth, is correct and consistent across your EHR and payer systems. This clean data upfront means smoother billing later.
What you get with Doctor Management Services:
- Fewer rejections caused by demographic errors
- Reduced administrative cost.
- Up to 30% increase in revenue.
- Accurate patient information synced across platforms
ICD, CPT, and HCPCS Coding
Our AAPC-certified coders know the difference between similar procedures and how each one should be reported. That’s why we ensure proper and accurate ICD-10, CPT, and HCPCS coding along with their modifiers.
We code every document properly, including injection, ablation, and nerve block, in alignment with payer rules and medical documentation. That’s how we help you capture every dollar you’ve earned while staying fully compliant.
Charge Posting
Missed charges? With GPA Consultancy, every charge is posted on time.
Our billing specialists post charges directly from your operative and clinical reports, double-checking for completeness. Whether it’s an E/M visit, post-op follow-up, or multi-level procedure, nothing slips through our system.
Our professionals work in detail to ensure an accurate charge posting keeps your revenue predictable and your billing cycle smooth.
Claims Submission
Speed and accuracy go hand in hand here at Doctor Management Services. We submit clean claims both electronically and one paper-based, usually within 24 hours of charge posting. Each claim is verified for coding errors and modifier accuracy before it ever reaches the payer. The result? Faster payments and far fewer denials to chase down later.
A/R Follow-Up
A/R follow-up is where many practices lose momentum and money. Our A/R team tracks every unpaid claim and follows up relentlessly until the balance is cleared. We review payer and insurance feedback thoroughly, identify recurring issues, and refile corrected claims quickly.
Because you should be paid for every service you provide.
Payment Posting
We make sure that no payment slips through or go in vain. Firstly, we record insurance payments, patient co-pays, and adjustments in real time. We have a dedicated verification team that then verifies each entry against the Explanation of Benefits (EOB) to ensure accuracy. With us, you’ll always know what’s been paid and what’s pending.
Reporting & Analytics
We believe that you should know what is going on with your claims. That is why our customized reports give you clear insights into collection trends, denial patterns, and payer performance. Now, no confusing spreadsheets, just straightforward billing reports that help you see how your practice is performing and where you can optimize and increase financial growth.
You’ll know exactly how our billing process improves your bottom line, month after month, with our medical billing service California.
Expanded Services for Various Specialties
In addition to our comprehensive services, we also offer specialized medical billing solutions for various medical specialties to ensure accuracy and efficiency. Our specialty-specific billing services include:

Cardiology Medical Billing Services
Accurate coding and billing for cardiology procedures and treatments to maximize reimbursements and reduce denials.
Chiropractic Medical Billing Services
Tailored solutions for chiropractic practices to handle unique billing challenges and improve cash flow.
Endocrinology Medical Billing Services
Expertise in billing for endocrine system treatments, ensuring compliance and optimal revenue recovery.

Gastroenterology Medical Billing Services
Specialized billing for gastroenterology procedures, enhancing claim accuracy and reducing payment delays.

General Surgery Medical Billing Services
Comprehensive billing services for surgical practices, focusing on precise coding and timely reimbursements.

Oncology Medical Billing Services
Specialized billing for oncology treatments, ensuring accurate claim submissions and optimal revenue.
Orthopedic Medical Billing Services
Expert billing for orthopedic services, from surgeries to physical therapy, improving financial performance.

Pathology Medical Billing Services
Efficient billing for pathology services, ensuring accurate claim processing and timely payments.

Pediatric Medical Billing Services
Dedicated billing solutions for pediatric practices, handling the complexities of child healthcare billing.

Physician Medical Billing Services
Comprehensive billing services for physicians, focusing on maximizing revenue and reducing administrative burdens.

Psychiatry Medical Billing Services
Tailored billing for psychiatric services, ensuring compliance with mental health billing regulations.
Radiology Medical Billing Services
Expert billing for radiology services, enhancing claim accuracy and accelerating payment cycles.
Urology Medical Billing Services
Specialized billing for urology practices, improving revenue cycle management and claim success rates.

EMR Medical Billing Services
Integration of billing with EMR systems, ensuring seamless data flow and accurate claim submissions.

Doctors Medical Billing Services
Comprehensive billing solutions for doctors, optimizing revenue cycles and reducing operational costs.
Schedule a free consultation to learn more
Complete the form and someone from our team will be in touch with you!
Our Stats
The Results Will Amaze You
Collection Rate
Claims Managed
$18.6 M
Revenue Recovered
30 Days
Average Case-to-Cash Time
Higher approvals on contested claims with expert follow-ups and negotiation.
What Doctors Say About Us
Working with them has been outstanding. Their branding, website design, and full digital strategy gave our practice a fresh, professional identity. Their knowledge of healthcare marketing for clinics helped us grow faster and reach more patients.
Excellent service and branding support. Our clinic’s online presence improved significantly and patient inquiries doubled.
Very professional team. They helped us scale our hospital marketing and website beautifully.

FAQs:
How does accurate medical coding impact reimbursement?
Accurate CPT, ICD-10, and HCPCS coding directly determines reimbursement success. Even a single incorrect code, modifier, or sequence can trigger automatic denials or underpayments. Our certified coders ensure every diagnosis and procedure code aligns with payer-specific requirements and US standards, maximizing claim acceptance on the first pass.
What makes your billing process different from typical billing companies?
Most billing vendors only submit claims; we manage the entire revenue cycle. From documentation review and code validation to payer follow-up, denial resolution, and reporting, every stage is handled with precision. Our Medical billing services California include a process that integrates compliance checks, root-cause denial tracking, and detailed payer rule mapping, ensuring your billing is both compliant and profitable.
How do I find the best medical billing services for my practice?
The best medical billing services combine precision, transparency, and advanced technology. When outsourcing, check whether they have a strong first-pass claim approval rate and proven expertise in your specialty.
Can you help resolve coding-related claim denials?
Absolutely, as one of the best medical billing and coding companies in USA, we help you navigate claim denials. We perform denial pattern analysis to identify root coding errors, such as invalid code combinations, missing modifiers, or outdated CPT updates, and then correct, refile, and appeal claims with proper documentation. This approach routinely increases recovered payments by 20–40%.
What’s included in medical billing and coding services?
Comprehensive medical billing and coding in the USA cover charge entry, coding compliance, claim submission, A/R follow-up, payment posting, and patient statement processing, all designed to improve efficiency and revenue.
How do you ensure compliance with CMS and AMA coding standards?
Our medical billing management services workflow is built around CMS and AMA regulations. Every claim passes multiple validation layers from code-to-diagnosis accuracy to payer policy verification. We also run periodic audits to maintain full compliance with HIPAA, HITECH, and California Medical Board requirements.
Do you manage documentation and coding audits for providers?
Yes, we are a medical billing and coding company in California that manages complete administrative tasks for healthcare providers. Our medical billing service California, conducts detailed pre- and post-submission coding audits to detect discrepancies, outdated codes, and missing documentation. These audits improve compliance, reduce denials, and protect providers during payer or state-level reviews.
Can you handle multiple specialties under one practice?
Yes, our system supports multi-specialty configurations from pain management, orthopedics, and neurology to surgery and diagnostic imaging. Each specialty is assigned dedicated coders trained in its specific billing nuances, ensuring accurate charge capture and faster reimbursements.
What is your process for claim follow-up and denial management?
As one of the top medical billing companies in California, we track every claim from submission to final payment. Denied claims are analyzed for root cause, corrected immediately, and appealed within payer deadlines. Regular denial reports help identify recurring issues and improve future clean-claim rates.
Can your team identify and fix revenue leakage?
Yes, our medical billing management services include regular audits and use claim-level analytics to detect missed codes, unbilled services, and underpayments. As a medical billing and coding company in California, we correct them at the source, improving cash flow and closing gaps that often go unnoticed in traditional billing setups.
Maximize your services
with our Help
Blogs

How Medical Billing Services Improve Practice Revenue
Efficient medical billing plays a key role in improving cash flow for healthcare practices. With accurate claim submissions, faster reimbursements, and reduced denials, clinics can focus more on patient care while maintaining a healthy revenue cycle.

Why Online Reputation Matters for Healthcare Providers
A strong online presence helps build trust with patients and improves your clinic’s credibility. Positive reviews, professional branding, and active reputation management can significantly increase patient inquiries and strengthen long-term growth.

The Importance of Credentialing for New Practices
Proper provider credentialing ensures that healthcare professionals are enrolled with insurance networks and eligible for reimbursements. Timely credentialing helps new practices avoid delays in claims processing and start serving patients without interruptions.
