Get Credentialed. Get Connected. Get Paid.
Medical billing and credentialing services can feel like a lot when you’re already running a busy practice. The forms, the follow-ups, it all takes more time than it should. That’s why we handle it for you. We keep the paperwork moving, stay on top of approvals, and make sure nothing gets stuck in the process. Your practice stays steady and organized, your payments come in on time, and you don’t have to chase anything. You get to focus on your patients, while we quietly manage everything in the background.
Medical Credentialing Services
Your Trusted Partner In Medical Provider Credentialing Services and Enrollment
With Gpa Consultancy expedited credentialing services for providers and enrollment services, your healthcare organization can maintain high-quality care standards without unnecessary stress or delays.
Advanced Credentialing Solutions for Modern Healthcare Providers
Physician credentialing is verifying and assessing a physician’s qualifications, training, experience, and licensure to ensure they meet the standards required to practice medicine within a healthcare organization.
If you’re searching for a credentialing services company with over 12 years of nationwide experience, you’ve come to the right place.
At GPA Consultancy, we provide tailored provider credentialing services for healthcare organizations. Our services include automated verification, real-time updates, and personalized support. We make your operations smoother, saving you time and resources while ensuring compliance and accuracy

All Doctor Credentialing Services Under One Roof
Individual Practitioners & Physicians
Group Practices & Clinics
Hospitals & Surgical Centers
Dental Practices
Home Health & Skilled Nursing Facilities
Laboratories & Imaging Centers
RCM Services
Tired of Credentialing Delays? Let’s Fix That.
We Bridge the Gap Between Your License and Your Patients.
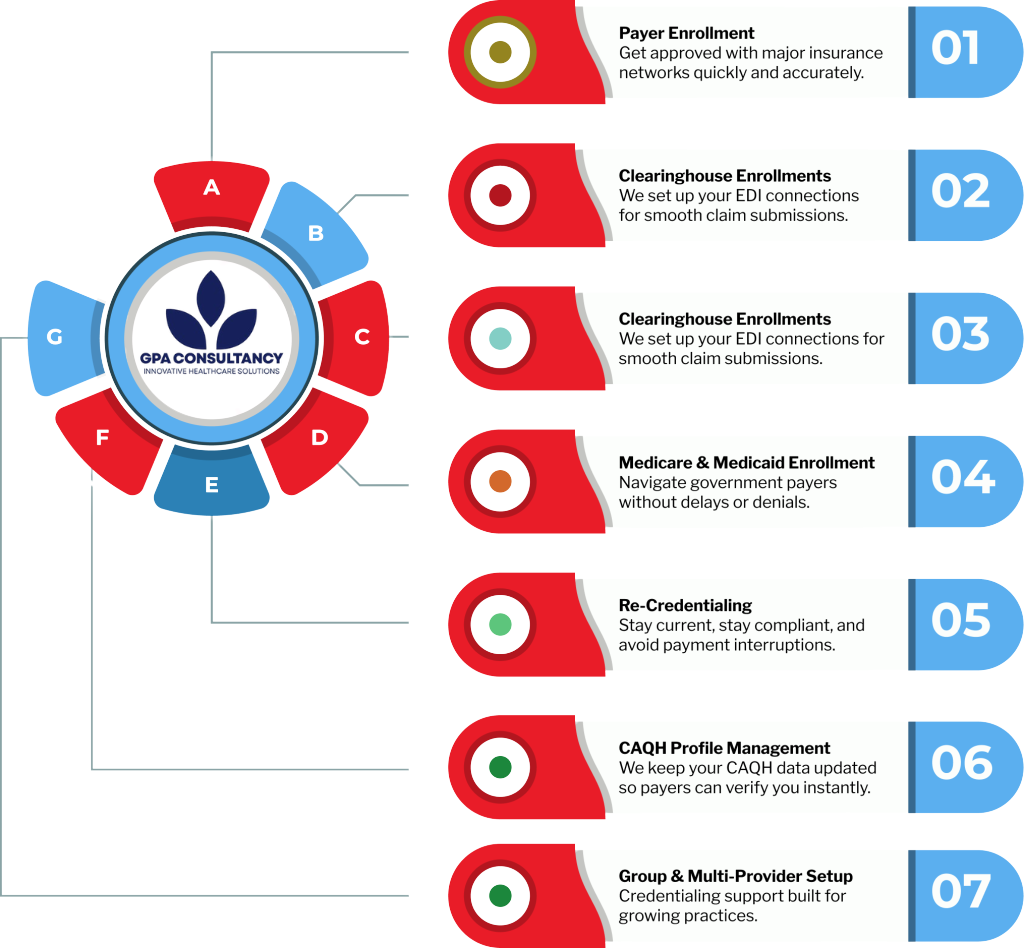
Here’s How We Make Credentialing Smarter for You:
Here is why more than 25000+ providers have trusted Doctor Management Services with medical credentialing services:
- 99.8% credential accuracy rate
- 95% reduction in manual data entry
- 99.9% data accuracy
- 80% reduction in credentialing admin costs
Reliable Support for Workers’ Compensation Billing Across All Types of Providers
Getting credentialed shouldn’t feel like a full-time job. From gathering documents to following up with payers. GPA Consultancy steps in to handle the details and make sure your applications move forward without unnecessary delays.
Enrollment & Setup
Credentialing Management
Advanced Credentialing
- New practices receive guidance on setting up credentialing from scratch, including payer applications and essential requirements.
- Partnering with reliable healthcare credentialing companies means your clinic gets consistent support, even during busy seasons.
- Multi-provider clinics benefit from a system that tracks every provider’s status, deadlines, and renewals in one place.
- As one of the experienced physician credentialing companies, we help reduce backlogs and prevent interruptions to your billing.
- Specialists get tailored support that fits their payer mix, state rules, and documentation needs.

State license application
U.S. DEA certificate
CLIA registration
- Tired of chasing state boards and waiting on endless approvals? Our medical billing and credentialing services handle the entire state licensing process in the USA from application to renewal across all 50 Medical and Osteopathic Boards. Whether it’s California’s Medical Board (MBC), Texas Medical Board (TMB), or New York’s OPMC, we take care of verifications, background checks, transcripts, and every board requirement
- Prescribers can’t afford downtime when it comes to controlled substances. Our physician credentialing service manages your DEA registration from start to finish, including Schedule II–V certifications, renewals, and address updates.
- Running lab tests? Our team of healthcare credentialing services helps you secure and maintain your CLIA certification under CMS and HHS guidelines. From initial registration to moderate or high complexity classification, we make sure your lab meets every federal and state quality standard; no inspection delays, no compliance surprises.
One Team for Every Type of Provider Enrollment in United States
End-to-End Revenue Cycle Management Services
Primary Source Verification
Provider Enrollment
We ensure accuracy and compliance with regulatory standards, as we authenticate education, training, licensure, certifications, and other relevant information directly from the issuing institution or authority.
Ongoing Monitoring and Re-credentialing
By proactively managing credentialing requirements and monitoring changes, we help healthcare organizations maintain regulatory compliance and streamline administrative processes.
Hospital Privilege Credentialing
GPA Consultancy provides comprehensive support for hospital privilege credentialing. Our expert team navigates credentialing requirements, expediting the approval process and enabling healthcare organizations to focus on delivering quality care without administrative burdens.
Provider Enrollment
We assist healthcare organizations and providers in the application process for various licenses essential for practice, including:
- Physician Licensing
- Non-Physician Licensing
- DEA Licensing
- CDS Licensing
- CLIA Licensing
- Group Licensing
Ongoing Monitoring and Re-credentialing
GPA Consultancy specializes in negotiating favorable payor contracts for healthcare organizations, leveraging industry expertise and data analytics to optimize reimbursement rates and contract terms.
Our Stats
The Results Will Amaze You
Collection Rate
Claims Managed
$18.6 M
Revenue Recovered
30 Days
Average Case-to-Cash Time
Higher approvals on contested claims with expert follow-ups and negotiation.
Transform Your Credentialing Process with Technology
GPA Consultancy CVO’s platform Incredibly puts large healthcare organizations in the driver’s seat of seamless credentialing. The Continuously Learning Platform, with Annual Major release updates is disrupting the way hospitals, clinics, etc, approach their credentialing processes. Here’s why:
Provider Onboarding Portal
GPA Consultancy in Credibly™ is a proprietary platform tailored to streamline the onboarding process for larger healthcare organizations. This innovative solution ensures swift and compliant onboarding of new providers, leveraging advanced features to enhance efficiency and accuracy throughout the entire onboarding journey.
- Azure Enterprise-Class Secure Cloud
- Real-Time Status Updates
- Expiration Alerts
- Secured Document Storage
- Automated Workflows
- Pre-populated Forms Library

Network Research
Recommendations on the most popular and effective in-network Payer mix for your group or practice.
Out-of-Network
Out of Network enrollments - Our team helps with NPI registrations on the Payer’s websites.
Closed Appeals
Requests for appeals on sometimes closed panels – while not guaranteed, we see a 35% success rate.
CAQH & PECOS Maintenance
We maintain and update your CAQH, PECOS profiles, making sure all information is accurate.
Demographic Update
Update a new TAX ID, address changes, bank account, and setting up of ERA and EFT enrollments.
Provider Roster Management
Maintain active providers and expiration management in a secured application.
Tailored Credentialing Solutions for Healthcare Organizations
Catering to larger healthcare organizations means being able to offer agility to adapt to their changing demands fast. After 12 years of servicing healthcare organizations nationwide, we have refined our offerings to cater to the diverse needs of our clients.

Pay Per Use
Start your credentialing journey with Gpa Consultancy CVO service. We handle new applications, demographic changes, portal verification, and maintain CAQH and PECOS.
This solution is efficient and comprehensive, designed for simplicity, and priced per transaction with a minimum commitment of $1,000.
Dedicated Team
Optimize your credentialing experience with a dedicated team exclusively committed to your Provider Onboarding, Primary Source Verification, Credentialing, Enrollment, and Maintenance needs.
This solution allows you to choose a customized scope that aligns with your specific requirements. With a commitment of at least 1 full-time equivalent (FTE), ensure a dedicated and efficient approach to your credentialing processes.
Analytics and Automation
Elevate your credentialing capabilities with Gpa Consultancy CVO’s Analytics & Automation capabilities.
This option makes your credentialing processes more advanced by providing custom reports for Management Dashboards using Power BI & Dataverse.
Benefit from seamless integration with EHRs like EPIC, eCW, Athena, AMD, ensuring a streamlined and efficient experience. Choose Gpa Consultancy for enhanced analytics and automation, transforming your credentialing insights into actionable intelligence.
What Doctors Say About Us
Working with them has been outstanding. Their branding, website design, and full digital strategy gave our practice a fresh, professional identity. Their knowledge of healthcare marketing for clinics helped us grow faster and reach more patients.
Excellent service and branding support. Our clinic’s online presence improved significantly and patient inquiries doubled.
Very professional team. They helped us scale our hospital marketing and website beautifully.

Medical Credentialing Expertise Across Diverse Specialties
For medical credentialing services in Houston,Texas or anywhere else in the USA, GPA Consultancy provides healthcare provider credentialing services for a multitude of specialties.
- Physicians
- Nurse Practitioners
- Physician Assistants
- Dentists
- Registered Nurses
- Licensed Practical Nurses
- Marriage and Family Therapists
- Dietitian/Nutritionists
- Physical Therapists
- Occupational Therapists
- Speech-Language Pathologists
- Clinical Psychologists
- Clinical Social Workers
- Chiropractors
- Optometrists
- Podiatrists
- Credentialing services for mental health providers

FAQs:
How do you manage CAQH and PECOS registration for new providers?
We create or update each provider’s CAQH and PECOS profiles, link their NPI and license details, and sync that information with payers to avoid enrollment delays. This ensures all data in both portals stays accurate and aligned with payer credentialing requirements.
What’s included in your NCQA compliance support?
Our credentialing company for physicians follows NCQA-approved verification procedures from primary-source checks to recredentialing reminders to keep your practice compliant with payer and accreditation standards. We also prepare you for NCQA or internal audits by maintaining documentation trails in real time.
How do you prevent data mismatches across credentialing systems?
Our team of doctor credentialing services makes sure to run automated cross-checks between CAQH, PECOS, and NPPES records to catch address, license, or taxonomy mismatches in credentialing services for providers before submission. This reduces payer rejections and keeps your medical credentialing records fully synchronized.
Can you handle credentialing updates for multi-state physicians or group practices?
Yes. Our medical credentialing services for providers cover single-state, multi-state, and multi-location setups. We track every board renewal, DEA registration, and state license update so your file stays active across all jurisdictions.
How often should my credentialing data be reviewed or revalidated?
We, as a medical credentialing company, recommend reviewing provider data every 90 days and performing full recredentialing every 2–3 years, depending on payer policy. Our platform automates these reminders, ensuring your physician credentialing stays current without interruptions.
What happens if a payer rejects an enrollment due to incomplete information?
Our team immediately audits the rejected application, fixes data errors, and resubmits it with the correct supporting documents. This minimizes lost time and ensures faster approval within insurance medical credentialing services workflows.
Do you assist with CAQH attestation and re-attestation reminders?
Absolutely. We monitor each provider’s attestation due date and handle re-attestation on schedule, keeping your CAQH file visible to payers at all times.
How do you ensure HIPAA compliance when managing credentialing data?
All documents are stored in encrypted, access-controlled systems with activity logs. Our credentialing company for physicians follows HIPAA’s Privacy and Security Rules, ensuring full protection of provider and patient-related data.
Can you integrate credentialing with my existing billing workflow?
Yes. Our medical billing and healthcare credentialing services are fully integrated credentialing data flows directly into payer enrollment and claim setup, preventing claim denials due to provider enrollment issues.
Are your credentialing operations based in California?
Yes. As one of the healthcare credentialing companies in California specializing in multi-specialty providers, we handle state-specific licensing, WC enrollments, and payer network setup for both individual doctors and group practices.
Maximize your services
with our Help
Streamline Credentialing: Stay Prepared, Avoid Disruptions
Why Choose GPA Consultancy for Physician Credentialing Services?
Our credentialing services for hospitals, groups, IPAs, and more ensure that healthcare providers are fully compliant with industry standards, streamlining the process for both new and existing staff members.

12+ Years Nationwide Experience

Efficient Provider Network Expansion

Round-The-Clock Availability

Scalable Services

RPA & API Proficiency

Flexible Pricing Options
Schedule a free consultation to learn more
Complete the form and someone from our team will be in touch with you!
Blogs

How Medical Billing Services Improve Practice Revenue
Efficient medical billing plays a key role in improving cash flow for healthcare practices. With accurate claim submissions, faster reimbursements, and reduced denials, clinics can focus more on patient care while maintaining a healthy revenue cycle.

Why Online Reputation Matters for Healthcare Providers
A strong online presence helps build trust with patients and improves your clinic’s credibility. Positive reviews, professional branding, and active reputation management can significantly increase patient inquiries and strengthen long-term growth.

The Importance of Credentialing for New Practices
Proper provider credentialing ensures that healthcare professionals are enrolled with insurance networks and eligible for reimbursements. Timely credentialing helps new practices avoid delays in claims processing and start serving patients without interruptions.
